Infection control and the use of disposable gloves
Principles
of glove use
Gloves are not a substitute for hand hygiene and should only be
used when appropriate. Their prolonged and unnecessary use may cause adverse
reactions and skin sensitivity and may lead to cross-contamination of the
patient environment. Inappropriate use of gloves can also undermine
hand-hygiene initiatives (Royal College of Nursing, 2017) and may be
distressing to patients (Nicklinson, 2011).
Indications for glove use and when to
wear gloves
- When
anticipating contact with blood or another bodily fluid
- As part of
transmission-based precautions (contact, airborne or droplet precautions)
where local policy requires this
- When anticipating
contact with chemical hazards, e.g. disinfectants/preserving agents
- When handling
sharps or contaminated devices (Loveday et al, 2014)
- When
undertaking an aseptic non-touch technique procedure – sterile/non-sterile
gloves chosen in line with procedure and local policy
Any cuts/abrasions on hands should be covered with
a waterproof dressing before gloves are donned
When to remove gloves
- As soon as
gloves are damaged (or non-integrity suspected)
- When contact
with blood, another bodily fluid, non-intact skin and mucous membrane has
occurred and ended
- When contact
with individual patients and their surroundings, or a contaminated body
site on a patient has ended
- When there is
an indication for hand hygiene
- When contact
with chemicals has ended
- After
completing an aseptic non-touch technique
Sources: Royal College of Nursing (2018), Loveday
et al (2014)
Gloves are single-use items and must be removed and
disposed of immediately after the care activity for which they have been worn;
they should not be washed or decontaminated with alcohol-based handrub as a
substitute for changing them between care activities. Hands must be
decontaminated after glove removal as there is evidence that hands become
contaminated:
- When
clinical gloves are worn – even when the integrity of the glove appears
undamaged;
- During
glove removal (Loveday et al, 2014).
Risk assessment
The need to wear gloves and the selection of appropriate gloves
requires an assessment of the task to be performed and its related risks to
patients and healthcare workers. Risk assessment should include consideration
of:
- Who
is at risk (patient or health professional);
- Whether
sterile or non-sterile gloves are required;
- The
potential for exposure to blood, bodily fluids, secretions and excretions;
- The
potential for contact with non-intact skin or mucous membranes during care
and invasive procedures;
- Health
professional and patient sensitivity to glove materials;
- Glove
size required;
- Organisational
policies related to a latex-free environment;
- The
potential for contact with hazardous substances such as chemicals, for
example cytotoxic drugs (RCN, 2018; Loveday et al, 2014).
Selection
Gloves are available in a range of materials. The most commonly
used is natural rubber latex (NRL), due to its efficacy in protecting against
bloodborne viruses and properties that maintain wearer dexterity (Loveday et
al, 2014). However, the proteins found in NRL gloves can cause severe allergic
reactions in health professionals and patients with existing allergies, and
contact dermatitis and occupational asthma in sensitised individuals. Powdered
latex gloves increase this risk and should never be used; if NRL gloves are
used they should be low protein. Neoprene and nitrile gloves have similar
barrier performance to NRL and are superior to vinyl as such, they are good
alternatives, although nitrile may also lead to sensitivity reactions (RCN,
2017; Loveday et al, 2014). Contact dermatitis is classified as an industrial
injury; as such, the Reporting of Injuries, Diseases and Dangerous Occurrences
Regulations 2013 (RIDDOR) requires a referral to occupational health if gloves
are causing a skin problem (Health and Safety Executive, 2013).
Medical gloves are categorised as non-sterile examination and
sterile procedure gloves; Box 2 lists the indications for glove selection.
Glove selection
Sterile gloves needed
- Any surgical
procedure
- Vaginal
delivery
- Invasive radiological
procedures
- Performing
vascular access and procedures
- Preparing total
parenteral nutrition and chemotherapeutic procedures
Examination gloves needed
Direct patient exposure
- Contact with
blood, mucous membrane and/or non-intact skin
- Potential presence
of highly infectious and dangerous organisms
- Epidemic or
emergency situations
- Intravenous
insertion or removal
- Drawing blood
- Discontinuation
of venous line
- Pelvic and
vaginal examination
- Suctioning
non-closed systems of endotracheal tubes
Indirect patent exposure
- Emptying emesis
basins
- Handling/cleaning
instruments
- Cleaning spills
of bodily fluids
Gloves not indicated (except for contact
precautions)
Direct patient exposure
- Taking blood
pressure, temperature and pulse
- Performing
subcutaneous and intramuscular injections
- Bathing and
dressing the patient (unless there is a risk of contact with bodily
fluids)
- Transporting
the patient
- Caring for eyes
and ears (without secretions)
- Vascular line
manipulation in absence of blood leakage
Indirect patient exposure
- Using the
telephone
- Writing on the
patient chart
- Giving oral
medication
- Distributing/collecting
a patient’s food tray
- Removing/replacing
a patient’s bed linen
- Placing non-invasive
ventilation equipment and oxygen cannulas
- Moving patient
furniture
- Using an
electronic care-recording device
Source: Adapted from World Health Organization
(2009)
The
procedure
Applying gloves
Gloves should be donned immediately before the intervention for
which they are required.
1.
Perform
hand hygiene.
2.
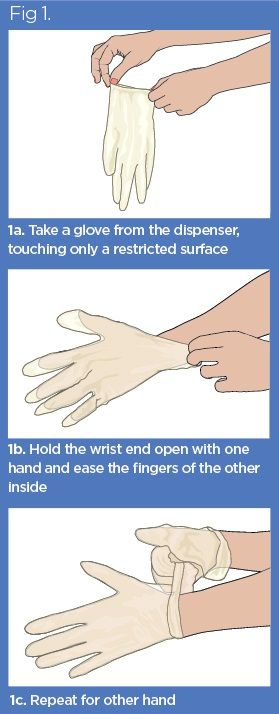
Take
a glove from the dispenser or package, touching only a restricted surface at
the wrist end (Fig 1a).
3.
Holding
the wrist end open with one hand, ease the fingers of the other hand inside.
4.
Gently
pull the wrist end of the glove while easing the hand into the glove, taking
care not to overstretch the material (Fig 1b).
5.
Taking
a second glove with the bare hand, turn the external surface of this glove onto
the gloved fingers at its opening. Ease the glove onto the hand (Fig 1c). This
avoids touching the skin with the gloved hand.
Once gloved, hands should not touch anything that is not defined by indications and conditions for glove use.
Source: Peter Lamb
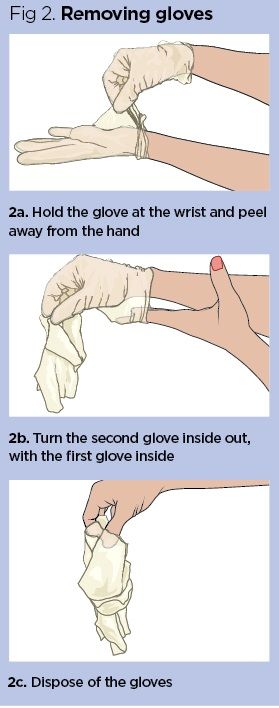
Removing
gloves
To avoid contaminating the hands or environment, gloves should
be removed carefully as soon as the intervention is complete; if a disposable
apron is also used gloves should be removed first (Loveday et al, 2014).
- Pinch
one glove at the wrist without touching the skin of the forearm and peel
away from the hand (Fig 2a), turning the glove inside out. Hold the
removed glove in the gloved hand.
- Hook
the index and middle finger of the bare hand inside the remaining glove,
taking care not to touch the outside of the glove (Fig 2b). Pull off the
glove, turning it inside out with the first glove inside (Fig 2c).
- Dispose
of the gloves in a clinical waste bin or, if contaminated with blood or
bodily fluids, into a hazardous waste bin.
- Perform hand hygiene.
Source: Peter Lamb
